Category:
Posted on November 18, 2024
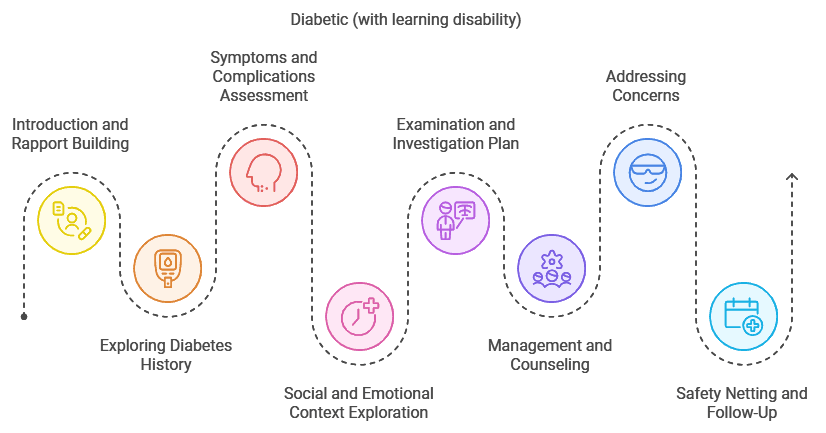
Managing a diabetic review for a patient with a learning disability requires clear communication, empathy, and a structured approach. This station tests your ability to explore the patient’s concerns, assess diabetic control, and provide tailored advice while considering their unique challenges. This guide will help you navigate the station confidently and effectively.
Begin by introducing yourself and confirming the patient’s identity:
“Hello, I’m one of the doctors here at the GP clinic. Am I speaking to Matt?”
Confirm their details:
“Can I get your full name and date of birth, please?”
Establish a comfortable pace and reassure the patient:
“It’s great to see you here for your diabetic review. Let’s go through things at your own pace.”
Use open-ended questions to explore their understanding of diabetes and treatment:
“For how long have you been diagnosed with diabetes?”
“What treatment are you currently taking?”
“Do you follow the doctor’s advice on how to take your insulin?”
Clarify and correct any misconceptions gently:
If the patient states incorrect insulin timing (e.g., “I take it after sugary food”), explain: “It’s important to take insulin regularly before meals to keep your blood sugar controlled.”
Assess their challenges:
“Do you sometimes forget your insulin dose?”
“Are you able to check your blood sugar regularly?”
“Do you know how to adjust your insulin doses if needed?”
Explore current symptoms related to diabetes:
“Have you noticed feeling excessively thirsty?”
“Do you urinate more often than usual?”
“Have you experienced any weight loss?”
Screen for complications:
Vision issues:
“Any problems with your vision?”
Numbness or tingling:
“Any unusual sensations in your hands or feet?”
Chest symptoms:
“Any chest pain or feeling like your heart is racing?”
Hypoglycemia:
“Do you ever feel dizzy or about to pass out after taking insulin?”
Understand the patient’s social support and living situation:
“Who do you live with?”
“Do you have family nearby?”
“What do you do for a living?”
Address emotional concerns:
“How have you been feeling lately?”
“Do you feel stressed or worried about managing your diabetes?”
For learning disabilities, probe gently:
“You mentioned getting confused with your insulin dose sometimes. Can you tell me more about that?”
Explore possible difficulties, such as:
Forgetting doses or instructions.
Difficulty understanding medical advice.
Pain from frequent injections.
Perform a general physical examination:
Check vitals, BMI, and inspect feet for diabetic complications.
Measure blood sugar levels during the visit.
Plan routine investigations:
Blood tests: HbA1c, cholesterol, kidney, and liver function.
Urine tests: Check for microalbuminuria.
Address the patient’s challenges with tailored advice:
Insulin Doses:
“You need to take insulin three times a day before meals and once at bedtime. How about we set reminders for you?”
Suggest notes, phone alarms, or help from family members.
Hypoglycemia Management:
“Always keep something sugary with you, like glucose tablets or juice, in case you feel dizzy after insulin.”
Diet and Exercise:
“A healthy diet and regular exercise like walking or swimming can help control your blood sugar and reduce stress.”
Provide additional support:
“We can arrange for a diabetic nurse to visit you regularly and help you manage your insulin.”
Offer a medical bracelet:
“This will let others know you’re on insulin in case of emergencies.”
Reassure the patient:
“It’s common to feel stressed about managing diabetes, but you’re doing a good job by coming for your review.”
Educate about the risks of uncontrolled diabetes:
“High blood sugar can damage your heart, kidneys, eyes, and nerves. Missing insulin doses can also lead to DKA, like what happened before.”
Encourage them to ask questions:
“Is there anything else you’d like to discuss today?”
Provide clear safety-netting advice:
“If you experience symptoms like severe dizziness, chest pain, or vision problems, please contact us or visit the hospital immediately.”
Arrange regular follow-ups:
“We’ll schedule follow-ups to monitor your progress and make sure you’re managing well.”
This station emphasizes empathy, patient education, and addressing individual challenges. By tailoring your communication and providing practical advice, you can confidently handle diabetic review cases, ensuring the patient feels supported and empowered to manage their condition.

Become part of a platform crafted by doctors who've been in your shoes and know what it takes to pass PLAB 2. Don't miss your chance to practice smarter and get ahead.
✓ No credit card required • ✓ Instant access • ✓ Made by doctors